Non Invasive Prenatal Care
Cell Free DNA Test – NIPT
Prenatal diagnosis includes all possible methods of population diagnosis and screening, whereby it is possible to detect or rule out chromosomal, structural, genetic, and functional abnormalities and fetal lesions. To achieve these goals, there are currently invasive and non-invasive methods available to the medical world from the first to third trimester of pregnancy.
Interventional diagnostic methods include:
- Chorionic villus sampling (CVS)
- Amniocentesis
- Fetal blood sampling
- Fetoscopy
Non-invasive methods on the other hand include:
- Ultrasound testing for the diagnosis of morphological abnormalities of the embryo, the detection of indicators of chromosomal abnormalities, and the monitoring of embryonic development.
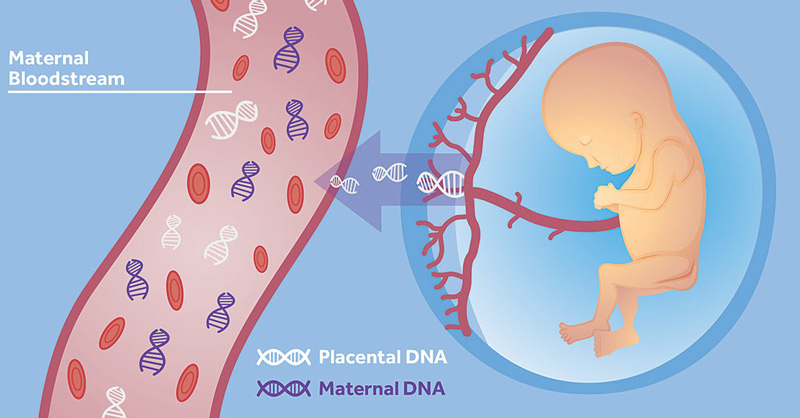
- Search for fetal cells or embryonic DNA in the mother’s blood (cell-free DNA).
When is CVS or amniocentesis appropriate?
Both are prenatal diagnostic methods and are recommended by doctors when there is an increased risk of chromosomal abnormalities such as Down syndrome, congenital abnormalities of the fetus, in cases of chromosomal abnormalities in the family, as well as for the diagnosis of conditions such as sickle cell anemia, cystic fibrosis, metabolic diseases, and infections.
CVS is mainly performed in the first trimester, up to the 14th week, while amniocentesis is performed after the 16th week of pregnancy.
What are the complications?
Randomized studies have shown that the rate of miscarriage after trophoblast (CVS) sampling is the same as fetal loss after second-trimester amniocentesis. There was only one randomized study comparing the risks of amniocentesis with women who only had an ultrasound. According to this study (Tabor 1986), the rate of miscarriage after amniocentesis was 1% higher. Today, the rate of miscarriage from invasive procedures is described as much lower, 0.1% – 0.3%.
Is the mother’s age indicative of amniocentesis?
Reproductive age over 35 years does NOT in itself constitute an indication for amniocentesis, since with it as an indication, we can diagnose only 30% of embryos with Down syndrome with a false-positive rate of about 5%. Therefore, if we perform amniocentesis based solely on the mother’s age, we would need to perform 140 amniocenteses to find one child with Down syndrome or risk losing one normal embryo for every two embryos with Down syndrome.
What is Cell Free DNA Test?
It has been discovered that a blood sample taken from the mother after the 10th week of pregnancy includes about 10% fetal DNA. With advanced molecular analysis methods, we can now reliably detect the most frequent trisomies (chromosomal abnormalities with more chromosomes than normal, such as Down syndrome, Edward’s syndrome, and Patau syndrome) with detection rates of > 99%, 97%, and 92%, respectively (cell-free DNA).
What are the benefits of this test?
- It is a non-invasive test since only a few ml of venous blood from the mother is needed.
- There is no risk of miscarriage.
- It has high diagnostic accuracy since it can diagnose >99% of Down syndrome babies, 97% of babies with Trisomy 18, and 92% of babies with Trisomy 13.
- False-positive results are 0.08%, 0.15%, and 0.2% for Trisomies 21, 18, and 13, respectively.
- It is applicable to single and twin pregnancies.
- It can be used in pregnancies achieved through in vitro fertilization (IVF) even in cases of donor eggs.
- With the introduction of new technology (NGS), information can be obtained about some microdeletion syndromes and sex chromosome abnormalities with or without further analysis of additional chromosomes (RATs).
Is it a diagnostic test?
Non-Invasive Prenatal Care is not a diagnostic method but a screening test with the highest accuracy so far, compared to the conventional prenatal combination of 1st and 2nd trimester.
To which women is the test applicable?
Non-Invasive Prenatal Testing is not a diagnostic method but a screening test with the highest accuracy so far, compared to the conventional combined prenatal screening of the 1st and 2nd trimesters.
To which women is the test applicable? This test can be applied to pregnant women and is proposed as an option for couples who want a harmless test to reassure them about the well-being of the fetus, excluding 97% of the most common chromosomal abnormalities (trisomies 21, 18, 13).
- For women who are at increased risk of having a baby with a chromosomal abnormality based on nuchal translucency (risk > 1/100) but less than 1/10.
- For women with an intermediate low risk of having a baby with chromosomal abnormalities (risk 1/101 – 1/2500).
- For women with a previous history of pregnancy with a chromosomal abnormality.
- For women with high-risk pregnancies potentially at risk of miscarriage from an invasive test (amniocentesis, CVS), such as in cases of first-trimester hematoma/vaginal bleeding/multiple pregnancies.
How is the test performed?
An ultrasound examination of the fetus is always required to record fetal cardiac function and exclude structural abnormalities. Immediately afterward, a blood sample is taken from the mother and sent to the relevant laboratory for testing.
When can the cell free DNA test be performed?
The test is proposed to be carried out from 10 to 40 weeks of gestation, with the ideal time being the 12th week during the nuchal translucency examination, so that the couple knows the results early, as well as the recombined final risk for chromosomal abnormalities.
When do we expect to have the results?
The results from the test are usually ready within 5 to 15 days, and the couple is informed immediately via a phone call.
Is there always a result?
In 1% of the cases, there is no result from the test, and this is due to a technical error in the analysis of the sample (e.g., a small percentage of fetal DNA in the mother’s blood). In this case, the couple is called to repeat the test for free, and the new results are expected, which will be obtained in about 50% of cases due to the previous failure of the analysis.
How are the results interpreted? What are the new data for the correct interpretation of the result?
The result we get is either low risk (good result) or increased risk (bad result).
A low-risk result means that the risk of chromosomal abnormalities from the nuchal translucency examination decreases even further in relation to the fetal fraction percentage of fetal DNA. Therefore, we now know how important the percentage of fetal DNA recorded in the result is, as well as the initial risk that the pregnant woman has from the nuchal translucency examination.
The greater the fetal fraction, the greater the risk reduction, with the maximum reduction noted with a fetal fraction >9%.
It is a screening test and not a diagnostic test. Therefore, in the case of increased risk, a diagnostic test (amniocentesis, CVS) is required to verify the result.
It is not recommended to identify sex chromosome abnormalities and RATs from the test, as there are many false-positive results, and there are no documented studies and safe methodology.
Are any additional tests / ultrasounds needed?
The cell-free DNA test does not provide information about other rare chromosomal abnormalities. If the ultrasound at 11-14 weeks shows an elevated nuchal translucency (more than 3.5mm) or major structural abnormalities in the fetus such as omphalocele, holoprosencephaly, heart abnormalities, or megacystis, then the risk for some rare chromosomal abnormalities becomes high. In such cases, a diagnostic test (amniocentesis, CVS) is recommended.
The cell-free DNA test does not provide information about structural abnormalities of the fetus, such as heart or brain abnormalities and spina bifida or information on fetal development. Therefore, it is advisable to have ultrasounds at 12 weeks, 20-22 weeks to look at fetal anatomy, and at 32 and 36 weeks to evaluate fetal development.


